Medical care for transgender and gender nonbinary people varies in accessibility and practice throughout the country.
At Colorado State University’s Health Network, it’s become more mainstream.
Dr. Cherie Worford is the clinical supervisor of the Women’s and Gender Care Clinic at CSU’s Health Network and a medical physician subtrained in obstetrics and gynecology.
One of Worford’s primary duties is to aid transgender and gender nonbinary people interested in medically transitioning via hormone injections.
“Medical transition is for patients who are identifying as transgender and are looking to take medications to potentially cause some external changes, … aligning internal gender identity with external gender (appearance),” Worford said.
“We try to be as straightforward as possible. It’s available, we’re here to do it, we’re happy to see you. Let us know how we can help, all without making it an overly medicalized situation.” Dr. Cherie Worford, CSU Women’s and Gender Care Clinic clinical supervisor, medical physician
According to Worford, the general process begins with an introductory meeting in which the doctor and patient go over the patient’s general health history and things that could potentially affect them being on medications.
This is followed by a discussion of the patient’s history with gender dysphoria, internal distress caused when an individual’s gender identity differs from the sex they were assigned at birth, she explained.

During this conversation, the doctor and patient discuss what aspects of their gender identity they find dysphoric and what the patient hopes to gain from being prescribed hormones, Worford said.
This includes short- and long-term goals, where on the gender spectrum the patient wants to transition toward and what they may want to accomplish overall by medically transitioning, she said.
“CSU in general, as most clinics now — which is good — run on what’s called the informed consent model,” Worford said.
This model requires medical professionals to educate their patients on what medical procedures are and the benefits and the risks involved, according to Worford.
Due to this practice, patients know what it is they want and the effects the medical practices can have prior to consenting to taking medications, she said.
“I essentially talk to patients about … what this (process) is, what hormones are, this is what they do, these are the benefits we see, these are the potential risks (and seeing if people are) still interested in doing it,” Worford said.
According to Worford, medical professionals don’t have to be involved in counseling nor do hormone suppliers require the approval of a mental health provider for a patient to qualify for hormones.
Before the implementation of the Health Network’s current practices, a patient had to pass certain criteria to be approved for any method of medical transitioning. They had to live as their desired and identified gender for a year before they could get approved to transition. This came with a lot of psychological and social safety issues associated with it, Worford said.
According to Worford, some patients come in the first day, and they know exactly what they want. For others, it takes a couple appointments and consultations for them to think things through and decide if they want to proceed toward a hormone treatment or if they aren’t ready to take that step yet.
“We try to be as straightforward as possible,” Worford said. “It’s available, we’re here to do it, we’re happy to see you. Let us know how we can help, all without making it an overly medicalized situation.”
For a full gender transition, from start to finish, the process can take up to three to five years depending on how far into the transition the patient would like to go, according to Worford.
In transgender women, breast development may take a long time, while in transgender men, their voice may deepen quickly but their facial and body hair growth can take longer, she said.
For gender nonbinary individuals or those who’d like an androgynous appearance, it may take less time in total, Worford explained.
“We don’t question their motives. It’s a legitimate procedure, and we are providing a service without judgement.” -Dr. Paul Steinwald, Denver plastic surgeon
Prescribed hormone doses vary for each person and where on the gender spectrum they’d like to be. An increase in dosage doesn’t necessarily speed up the process. For some, it simply increases the symptoms, Worford said.
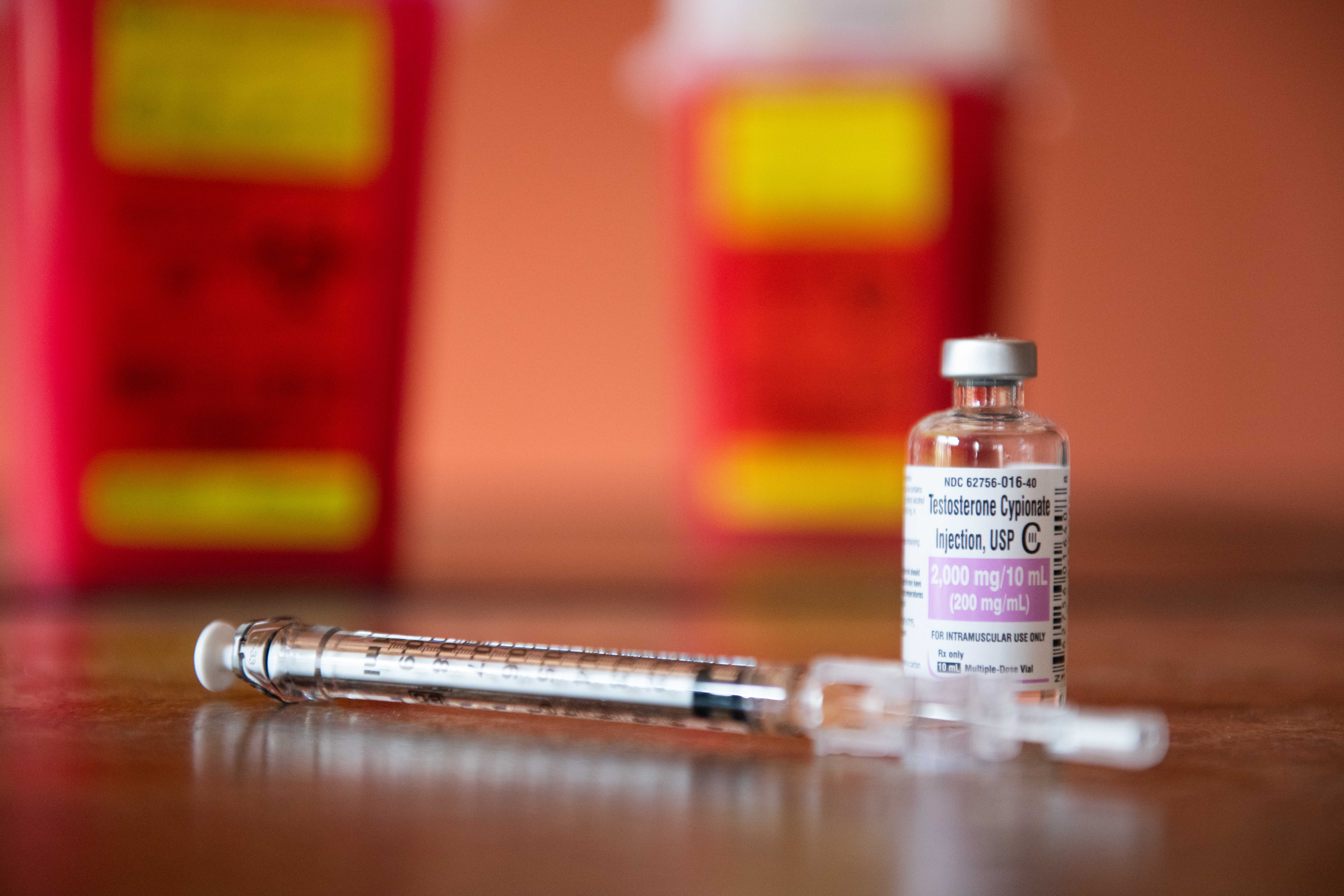
“It can be a slow process,” Worford said. “I tell people it’s a similar concept to puberty. For a majority of us, puberty does not happen overnight. … Most of us didn’t really enjoy it. It’s like a second puberty.”
Jill Vesty is a family nurse practitioner who works alongside Worford at the CSU Health Network. She aids in educating patients on the process of taking hormones, helping them decide what steps to take on their journey through transitioning.
Vesty has worked with the Health Network for 10 years and was on staff when it started to implement transgender health care.
“I care about people, I care about society,” Vesty said. “I think everybody deserves health care, and I want to help people access it.”
According to Vesty, the CSU Health Network has largely mirrored the type of care that has become more normalized throughout the United States for this community.
A type of health care that was once thought to be specialized, transgender care has become more incorporated into general, primary care, Vesty explained.
“I think it’s great when a transgender student can come in with any number of medical issues, … and the same clinician can manage all of those medical issues,” Vesty said. “It increases access if you have more general family practitioners … to provide this care as part of their routine.”
According to Vesty, this improves awareness across the spectrum and makes resources more widely known. This allows individuals who are on their way to transitioning to become aware of what is available, she said.
Vesty said the Health Network does not provide specialty care like plastic surgery. However, they are always able to recommend services that are both financially and regionally accessible for their patients.
Dr. Paul Steinwald is a plastic surgeon with the Center for Cosmetic Surgery, located in Denver. A specialty to his practice is his chest masculinization procedure, otherwise known as top surgery.
According to Steinwald, he is one of the few plastic surgeons that, when removing breasts, will try to keep the breast attached, specifically the nipple.
While this is considered to be a more difficult procedure that has risks, Steinwald said it is more likely to retain sensation in the area.
While other surgeons generally take the nipple off and graft it back on, Steinwald prefers to only do that for individuals with larger breasts, size DD or higher.
“It heals better than a graft ever would,” Steinwald said. “And you can adjust it or revise it later with everything still attached, versus grafting.”
According to Steinwald, it’s really about how the patient will scar. If the nipple looks good two weeks after the procedure, then the patient is in a good place. Otherwise, the need for revision would be considered.
Overall, it’s a very well-tolerated procedure with “a 95% success rate for nipple survival, and that’s key,” Steinwald said.
Steinwald has been working with the transgender community for the majority of his career, his first experience occurring in 2002.
“It’s a very wonderful population of patients,” Steinwald said. “I think they should be treated like everyone else, with good, safe care and respect.”
His staff has reported positively when working with individuals within the community.
“We don’t question their motives,” Steinwald said. “It’s a legitimate procedure, and we are providing a service without judgement.”
Dorina Vida can be reached at news@collegian.com or on Twitter @simply_she_.